Urothelial Carcinoma
What is Urothelial Carcinoma?
Urothelial Carcinoma is a multifocal malignancy associated with the reno-urinary system. Renal parenchyma often develops a high-grade scirrhous mass formation and turns to a malignant tumor. In urothelial carcinoma, the organ which can get affected with malignant attacks is renal pelvis, ureters, and bladder. The possibility of this organ get affected with Urothelial Carcinoma can be estimated as 1:3:50 respectively.
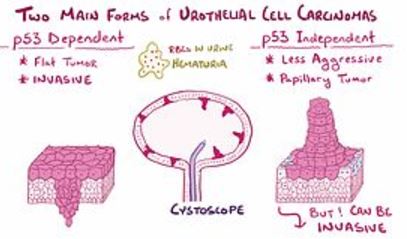
It has been observed that upper urinary tract cancer affected patients have a 30 to 50 percent tendency to develop bladder cancer, whereas bladder cancer affected individuals also has a 2 to 3 percent tendency to develop urinary tract cancer. Therefore, the reno-urinary system is interconnected and the scope of cancer progression also inter-related1,2.
Symptoms
Hematuria
Urothelial Carcinoma affected individuals often have blood in the urine (hematuria). The onset of hematuria usually not associated without pain, but the passage of urine is obstructed due to tumor location leads to arising of pain.
Urinary voiding symptoms
The urgency of urine passing, frequent urination, incomplete urine passage and/ or dysuria are all related to urinary voiding system. This symptom is common in patients having bladder and/or urinary tract malignancy, however, this symptom is less common in cancer originated at the renal pelvis.
Bladder irritation without hematuria
In the case of Urothelial Carcinoma originated from urinary bladder can cause vesical irritation without commencing hematuria.
Symptoms in advanced stage
With the progression of the Urothelial Carcinoma can cause fever, nocturnal perspiration, anorexia and weight loss. Pain in the lower limbs often common due to venous and lymphatic obstruction leads to edema1,3.
Causes
Some factors increase the risk of Urothelial Carcinoma. These factors are
Tobacco smoking
Tobacco containing cigarettes smoking is one of the causative factors for urothelial carcinoma. It has been observed that prolonged cigarette smoking and frequency of smoking is directly linked with incidence of Urothelial Carcinoma. Prolong frequent cigarettes smoking affects transitional cell and squamous cell lining of the reno-urinary system.
Analgesic abuse
Excess analgesic intake, specifically phenacetin-containing drug increase the risk of cancer in the reno-urinary system. Over-use of analgesic negatively affects the renal pelvis and renal papillary necrosis is one of the primary cause of cancer development.
Chronic urinary tract inflammatory condition
Urothelial Carcinoma is also an outcome of chronic urinary tract inflammatory condition. Stone formation in the upper urinary tract often leads to inflammation in the urinary tract. Chronic bladder infection also leads to inflammation and can manifest Urothelial Carcinoma.
Occupational hazardous
Hazardous exposure to toxic substances due to occupational reason also has a great role in the onset of Urothelial Carcinoma. The rubber, organic chemical and paint or dye industries are using different toxic materials which are harmful to reno-urinary system and workers who work in these industries have increased risk to develop Urothelial Carcinoma. It has been observed that aniline dye workers mainly develops Urothelial Carcinoma.
Balkan nephropathy
Balkan nephropathy affected patients have increased the risk of Urothelial Carcinoma development. Balkan nephropathy patients have progressive inflammatory condition affects the renal parenchyma, which leads to renal failure and gradually turns Urothelial Carcinoma by affecting the renal pelvis and ureters.
Genetic factors
It has been observed that some patients with Urothelial Carcinoma having familial history and that provide the possibility of involvement of the genetic factor in the case of onset of Urothelial Carcinoma1,3.
Prevalence
The prevalence of the Urothelial Carcinoma is more in men than women. The male incidence is thrice time higher than the female and usual onset is after 70 years of age of the individual. In addition, it has been also found that white race people have a greater risk than the black and the estimated ratio is 2:11,2.
Diagnosis
After initial physical examination and symptomatic discussion and medical history analysis, suspected cases require conducting several laboratory tests, including computed tomography [CT] scan, magnetic resonance imaging [MRI], and intravenous pyelogram. The abnormal report requires performing cystoscopy. For the confirmatory result, ureteroscopic examination and biopsy test are performed1,3,4.
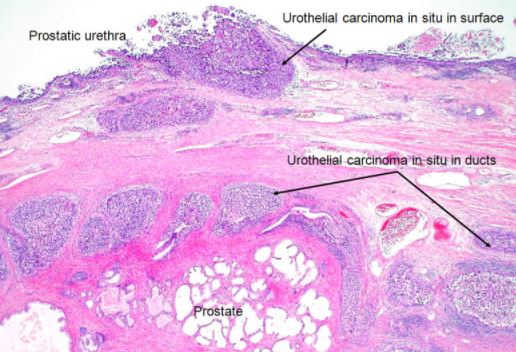
Treatment
Urothelial Carcinoma is treated with surgical intervention. The presence of cyst often requires Cystectomy. In addition, adjuvant therapy also added including radiation therapy3,4.
Prognosis & Survival Rate
The prognosis of the Urothelial Carcinoma depends upon the invasive nature of the malignancy and spreading of metastasizing. In the case of initial stage low-grade cancerous lesion provides a good prognosis, whereas poor prognosis is reported with the high grade cancerous lesion. The local invasion of the carcinoma can provide 5 years survival, whereas involvement of the lymph nodes can cause 0 to 30 percent 5 years survival1.
References
- Mark Hurwitz, Philippe E. Spiess, Jorge A. Garcia, Louis L. Pisters, Urothelial and Kidney Cancers. June 01, 2016. cancerNetwork. Online available at http://www.cancernetwork.com/cancer-management/urothelial-and-kidney-cancers
- David F Jarrard. Urothelial Tumors of the Renal Pelvis and Ureters. Sep 18, 2016. Medscape. Online available at http://emedicine.medscape.com/article/452449-overview#a8
- MARIANA DEACU, MĂDĂLINA BOŞOTEANU, MARIANA AŞCHIE, GABRIELA BĂLTĂŢESCU, V. SÂRBU, MARIANA BĂRDAŞ; Urothelial carcinoma of the renal pelvis associated with cystic disease of the kidney. Rom J Morphol Embryol. 2011;52(1 Suppl):497-501. Online available at https://www.ncbi.nlm.nih.gov/pubmed/21424101
- Rugvedita Parakh, Monika Roychowdhury, Bladder
Urothelial carcinoma-invasive
General. 18 July 2016. Online available at http://www.pathologyoutlines.com/topic/bladderurothelialinvasivegen.html
