Lamellar Ichthyosis
What Is Lamellar Ichthyosis?
Lamellar ichthyosis is a skin disorder that occurs at birth and can continue throughout life. It is characterized by redness and generalized scaling on the skin. This condition is not a threat to life but causes serious disfiguring of the skin of the affected person. This condition can cause significant stress to the affected person6.
Lamellar ichthyosis is a rare disorder and can affect both men and women equally. It also occurs in all ages and patients with this disorder lead a normal life.
However, once the child sheds off the membrane covering the body, he/she become vulnerable to secondary sepsis and hypernatremic dehydration. Sepsis is a serious condition where the immune system responds to an infection by attacking and destroying its own tissues and organs. Hypernatremic dehydration is a condition where the body has lost a lot of water compared to sodium levels.
Ichthyoses
Refers to a collection of skin disorders that are characterized by unusual buildup of squames (dead skin cells) on top of your skin.
Ichthyosis congenital
It is hereditary skin disorder. It causes the skin to become red, dry and rough with large bumpy and white scales. It can also make the soles of your feet and palms of the hand to become unusually thick.
X-linked ichthyosis
This is a hereditary skin condition that affects men more than women. This disorder leads to the formation of brown scales on your legs, back and backside of the neck.
Causes
Defective genes
The main cause of lamellar ichthyosis is abnormal genes that occur as a result of mutation of several genes. Genes that are responsible for this disorder include: genes that encode epidermal enzyme Transglutaminase 1 and those that encode 12(R)-lipoxygenase and lipoxygenase-3.
Transglutaminase 1 enzyme plays significant contribution during formation and maturation of the stratum corneum. The enzyme helps to cross-link epidermal proteins to support stratum corneum develop and mature.
These defective genes can be inherited recessively. In this case, for a child to have this disorder, both parents must have the mutated gene to pass to the child. If the child inherits a normal gene from one parent and a gene for this disorder from another parent, the child becomes a carrier for this condition but will not exhibit this disease.
When parents are carriers of this disease, they are also likely to the pass this disorder to the child.
Symptoms
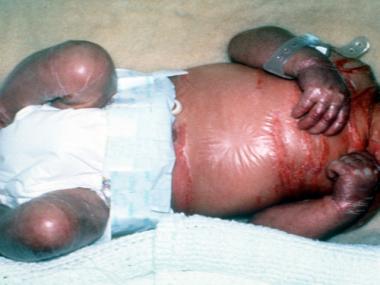
Lamellar ichthyosis occurs at birth. Many infants born with this disorder are covered with a transparent casing known as collodion. The skin of these affected babies is dark, red and appears split and tight. This skin will disappear after a few days when the baby is born.
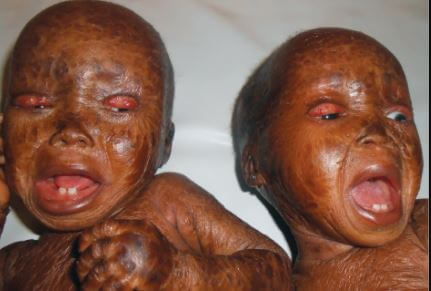
The tightness of the skin forces the lips and eyelids of the babies to remain open. The babies have difficult in closing their eyes. As the skin around the eyes pulls tightly, it forces the eyelid to turn out causing irritation in the eyes of babies, a condition known as ectropion.
When ectropion is not treated immediately, it will damage the cornea affecting vision in babies. In some babies, the area around their fingers can become hard due to tightening of the skin.
Other symptoms of this disorder include babies losing a lot of water and have difficult in controlling body temperatures. In some cases, babies can be infected from secondary and systemic infections such as sepsis.
Other babies with lamellar ichthyosis may have thick nails and lose hair due to thick scalp. Thick skin can also be noticed on the baby’s soles of the feet and palm of hands.
Diagnosis
Diagnosis of lamellar ichthyosis is based on clinical examination of patient’s skin. Your dermatologist examines your skin to identify dark, red and thick skin with scales.
Biopsy can be performed to determine the cause of this disorder. Your dermatologist will scrap a sample of your skin and analyze it in the laboratory to help diagnose lamellar ichthyosis.
Treatment
There is no treatment for Lamellar Ichthyosis. The main aim of treatment is to manage the symptoms and secondary infections. For severe symptoms of lamellar ichthyosis, your doctor can prescribe medications such as retinoids (isotretinoin).
Secondary infections
- Antibiotic drugs- These drugs are used treat infection caused by bacteria in your body.
- Vasoactive drugs- These medications help in rising blood pressure of the patient.
- Insulin- This will help to regulate the blood sugar of the patient.
- Corticosteroids-In case sepsis is causing inflammation in your body; this type of drug can help relieve inflammations.
- Surgery: Surgery intervention can also be used to treat sepsis infection. Surgery can be used to remove the affected tissue or drain out pus from a tissue.
Reduce sepsis infection by
- Ensure that you are regularly vaccinated for flu, pneumonia and other infections.
- Take good care of yourself by taking a bath regularly and washing your hands and caring for the wound properly.
- Seek for urgent medical help when you have an infection. Sepsis can be easily treated when it’s detected early.
Ectropion Treatment
Lubricating drops
- Your doctor can give you lubricating drops to help prevent the cornea from damage. You have to apply these drops by wiping your eyes from the external eye to the nose to prevent worsening the symptoms.
Surgery
Surgery can be effective in correcting cornea damage and prevent other eye complications. During surgery, patients are put under an anesthesia and the doctor removes the section of the lower eyelid. Stitches will be put under your eyelid or on the outer surface of your eye.
After surgery you will wear temporal eye patch. Your doctor will also administer steroid and antibiotics to prevent eye infections. In case of pain, you will be given painkillers.
You can enhance the appearance of your skin by regularly using moisturizers and bath oil. They help prevent cracking and dryness on your skin. Use massaging cream on your palms and below your eyes to prevent tightening of the skin6.
Pictures
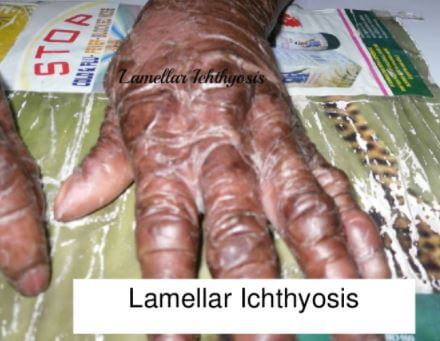
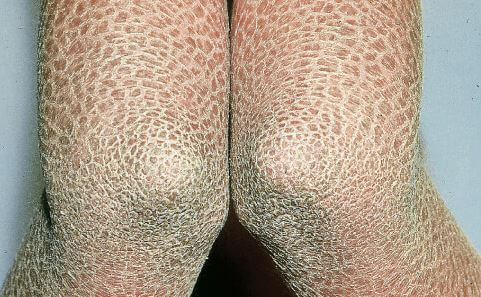
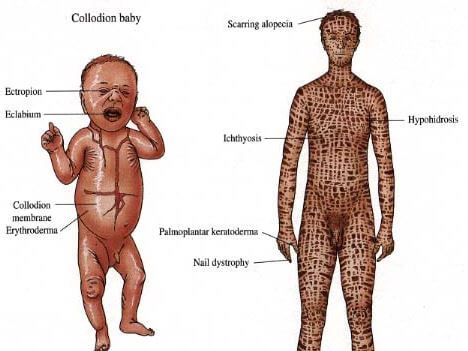
Reference List
- http://www.healthline.com/health/ectropion#treatment4
- Sepsis. Available at http://www.healthline.com/health/sepsis#recovery12
- Lamellar ichthyosis. Available at http://emedicine.medscape.com/article/1111300-overview#a2
- https://rarediseases.org/rare-diseases/ichthyosis-lamellar/
- http://www.ichthyosis.org.uk/lamellar-ichthyosis/
- https://ozarkderm.com/lamellar-ichthyosis
